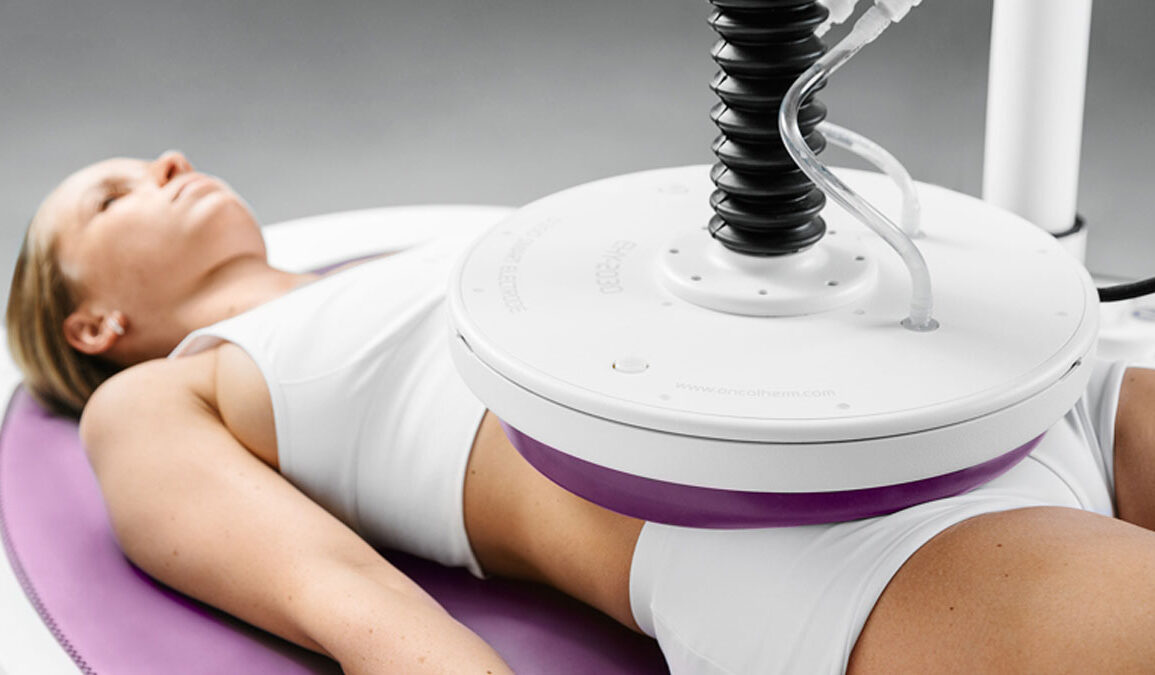
As triple-negative breast cancer continues to challenge doctors and patients with its aggressive nature and resistance to standard treatments, a centuries-old idea is gaining new ground: fight cancer with heat. From ancient Egypt to modern-day oncology labs, hyperthermia therapy—raising the temperature of cancerous tissue—has emerged as a promising tool in combination with other treatments to target stubborn tumors.
The Basics of Hyperthermia Therapy
Hyperthermia therapy involves heating body tissue to temperatures around 110°F (43°C). This can be done with hot water bags, microwaves, magnetic fields, or even nanoparticles designed to release heat when activated by light or electricity. The goal is to raise the temperature of the tumor while keeping nearby healthy tissue safe.
Dr. Jennifer Yu of the Cleveland Clinic, one of the doctors pioneering this approach in breast cancer care, explains: “Hyperthermia increases blood flow to the tumor and makes it more sensitive to radiation. It improves cell kill.” In one study, 66 percent of patients receiving both hyperthermia and radiation saw their tumors shrink completely, compared to 42 percent who received radiation alone.
Lisa Ridgeway, a mother of two battling triple-negative breast cancer, turned to this method after surgery, radiation, and chemotherapy failed. “My choice is I want to live,” she said.
The Science Behind the Heat
Hyperthermia doesn’t just cook the cancer, it activates the immune system. Heat disrupts proteins that help cancer cells repair themselves after radiation or chemo. It makes cell membranes more permeable, allowing drugs to enter more easily. It can also trigger a process called immunogenic cell death, where dying cancer cells release signals that attract and activate immune cells.
Researchers have shown that hyperthermia affects both the innate and adaptive immune systems. Neutrophils, dendritic cells, natural killer cells, and T-cells all become more active. Tumors that were previously “cold” (lacking immune cell activity) can become “hot,” meaning they’re now visible to and attacked by the immune system.
A recent review in Frontiers in Immunology stated, “Hyperthermia amplifies the efficacy of immune checkpoint inhibitors by improving immune cell infiltration and enhancing antigen presentation.”
Heat and Nanomedicine: A High-Tech Tag Team
The rise of polymeric nanomaterials (PNMs) has added precision to hyperthermia therapy. These tiny particles, designed to accumulate in tumors due to their leaky blood vessels, can be activated by light or magnetic fields to heat tumors from within.
Researchers report that combining photothermal therapy, photodynamic therapy, and hyperthermia into one nanostructure may “potentiate synergistic cytotoxicity while attenuating off-target toxicity.” In other words, more cancer cells die, and healthy cells are left alone.
These platforms also serve as drug carriers, releasing chemotherapy directly into the tumor once heated. The result is a highly targeted approach that combines heat, immune activation, and drug delivery in one treatment.
A New Ally: Ivermectin
In one recent animal study, scientists combined a special form of hyperthermia called modulated electro-hyperthermia (mEHT) with the antiparasitic drug ivermectin. The goal was to block heat-induced activation of a stress protein called HSPB1, which helps cancer cells survive heat. The result: significantly smaller tumors, more cancer cell death, and less tumor cell proliferation. Importantly, the treatment was well tolerated, with no major weight loss or toxicity in mice.
“IVM synergistically improved the tumor growth inhibition achieved by mEHT,” the researchers wrote, adding that ivermectin inhibited the phosphorylation of HSPB1, which appears critical in stopping cancer cells from repairing heat damage.
From Ancient Roots to Modern Clinics
Hyperthermia has deep historical roots. Ancient Egyptians used heat to treat breast cancer. Hippocrates noted that fever could help epilepsy, and in the 19th century, Dr. W. Busch observed cancer remission after a patient developed a high fever from infection.
Today, about 10 centers in the U.S., including Long Beach Memorial’s Todd Cancer Institute, offer hyperthermia for breast cancer. Treatments usually last an hour and are repeated weekly or biweekly.
Enhancing Standard Treatments
Hyperthermia works especially well when paired with radiation or immunotherapy. When combined with radiation, it improves oxygen flow to the tumor, enhances DNA damage, and increases immune cell infiltration. Radiation also makes tumors release immune-alerting molecules, further boosting the effects of heat.
Combining hyperthermia with immune checkpoint inhibitors has shown promising results in preclinical trials, especially for hard-to-treat tumors like triple-negative breast cancer and glioblastoma. Early clinical trials in lung, liver, and breast cancer are beginning to show better outcomes when hyperthermia is added to immunotherapy.
Transforming the Tumor Microenvironment
Cancer tumors often grow in oxygen-starved, immune-silent environments. Heat changes that. It boosts blood flow, raises oxygen levels, and activates immune cells. The result: tumors become more visible to the immune system. Pro-inflammatory cytokines like IL-6 and TNF-alpha are released, and suppressive cells like myeloid-derived suppressor cells decrease.
“HT can transform cold tumors into hot tumors by increasing immunogenicity, promoting dendritic cell activation, and remodeling the stroma,” researchers noted in Frontiers in Immunology.
Although the evidence is growing, more research is needed to fine-tune hyperthermia’s use in cancer care. Key questions remain: What’s the best way to deliver heat? Should it be localized or whole-body? How do we predict who will benefit most?
Still, experts are optimistic. As one review concluded, “Integrating hyperthermia into multimodal cancer therapy offers new therapeutic opportunities for patients with resistant tumors.”
For patients like Lisa Ridgeway, who had no good options left, hyperthermia offers something priceless: hope.