A growing body of research is raising serious concerns about a condition that millions of people may not even know they have. Obstructive sleep apnea, a disorder that disrupts breathing during sleep, is now being linked to bleeding in the brain and an increased risk of dementia. New findings suggest that what happens during the night could have lasting consequences for brain health years later.
What Is Sleep Apnea and Why It Matters
Obstructive sleep apnea is a common sleep disorder in which breathing repeatedly stops and starts during sleep. These interruptions reduce oxygen levels in the blood and fragment normal sleep cycles. Over time, this strain on the body has already been linked to high blood pressure, stroke, and cardiovascular disease.
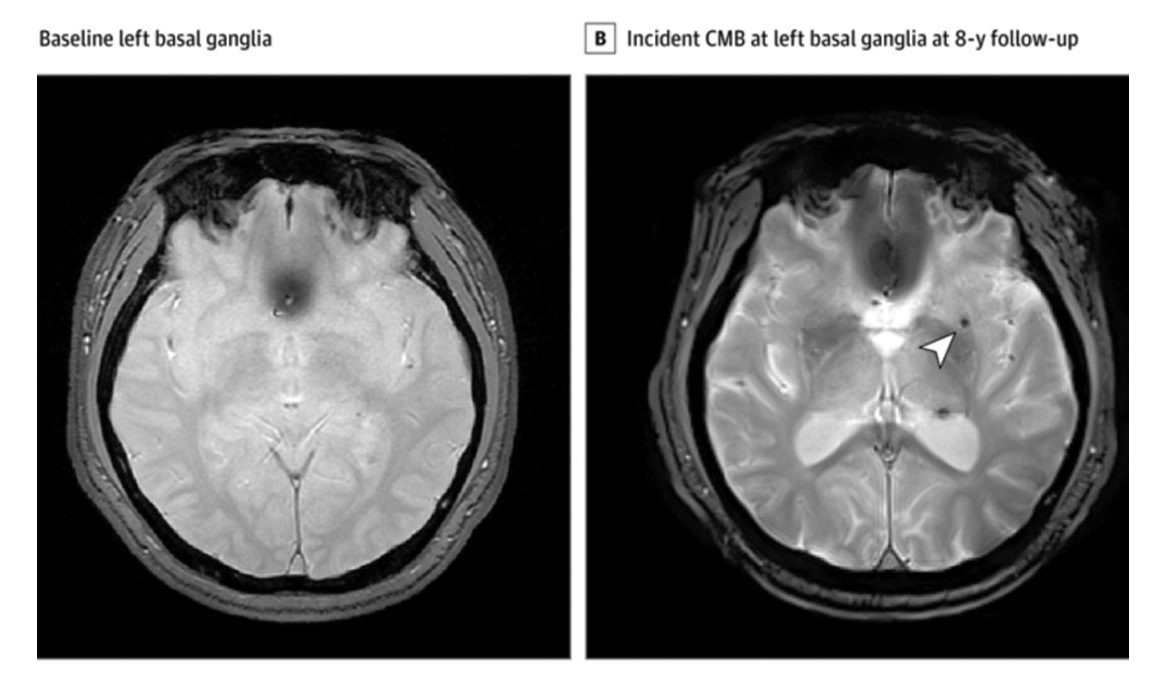
What is becoming clearer now is its impact on the brain itself. Researchers are increasingly focusing on how these repeated drops in oxygen may damage small blood vessels in the brain, leading to what are known as cerebral microbleeds. These are tiny hemorrhages that can only be seen on specialized brain imaging but are strongly associated with cognitive decline and stroke.
The Research Connecting Sleep Apnea to Brain Bleeding
A large Korean study followed 1,441 middle aged and older adults over eight years, tracking both their sleep patterns and brain health. Participants underwent overnight sleep studies and repeated MRI scans to detect changes in the brain.
The findings were striking. People with moderate to severe sleep apnea had more than double the risk of developing cerebral microbleeds compared to those without the condition. The relative risk was calculated at 2.14, even after adjusting for other factors such as age and genetic risk.
The numbers tell a clear story. After eight years, only 3.33 percent of people without sleep apnea developed microbleeds. That number was similar for mild cases at 3.21 percent. But for those with moderate to severe sleep apnea, the rate jumped to 7.25 percent.
Other studies reinforce these findings. In one clinical analysis, patients with higher apnea hypopnea index scores showed a significantly greater likelihood of brain microbleeds. Moderate to severe cases were identified as “an independent predictor of CMBs,” with an adjusted odds ratio of 4.51.
Researchers also found a direct relationship between the severity of sleep apnea and the number of microbleeds in the brain. In simple terms, the worse the apnea, the more damage was observed.
Why Brain Microbleeds Matter
Cerebral microbleeds are not harmless. They are considered an early warning sign of small vessel disease in the brain and are closely linked to both stroke and dementia. As these tiny hemorrhages accumulate, they can disrupt normal brain function and accelerate cognitive decline.
The implication is significant. Sleep apnea may not just affect how rested someone feels the next day. It may quietly increase the risk of long term neurological damage.
Researchers describe sleep apnea as a “modifiable risk factor,” meaning that identifying and treating it early could help prevent or reduce these outcomes.
The Role of Wearable Technology
With growing awareness, many consumers are turning to wearable devices to track their sleep. Devices like smartwatches and rings are becoming more sophisticated, and some can flag signs of severe sleep apnea.
However, the limitations are important. Studies show that common devices still fall short compared to clinical testing. Apple Watches, for example, have shown only about 50.5 percent sensitivity in detecting sleep stages, with significant inaccuracies in identifying both light and deep sleep.
Fitbit devices perform somewhat better, and Oura rings show stronger results, but none match the accuracy of professional sleep studies. More importantly, these devices struggle to reliably detect moderate sleep apnea, which is still associated with increased brain risk.
The takeaway is clear. Wearables can be a useful screening tool, but they are not a substitute for a formal evaluation by a sleep specialist.
What Can Be Done About Sleep Apnea
The good news is that sleep apnea is often treatable. The most widely used treatment is continuous positive airway pressure, or CPAP, which keeps airways open during sleep. Variations such as APAP and BiPAP adjust pressure levels to improve comfort.
Other options include oral appliances that reposition the jaw, lifestyle changes like weight loss and avoiding alcohol, and positional therapy to prevent sleeping on the back. In more severe cases, surgical interventions or implantable devices may be considered.
Still, treatment is not always easy. Roughly half of patients struggle to tolerate CPAP therapy due to discomfort, dry mouth, or mask fit issues. That has led researchers to continue exploring alternative approaches.
There are currently no medications that cure sleep apnea, although some drugs may be used to manage persistent daytime sleepiness.
What Experts Are Saying
Researchers emphasize that many people remain undiagnosed. One of the key warnings from recent studies is that “people don’t always know they have it,” even as damage may already be occurring.
The emerging consensus is that screening should become more common, especially for middle aged and older adults or those with cardiovascular risk factors. Early detection could play a major role in preventing long term brain damage.
The broader conversation around public health is beginning to include sleep disorders as a serious risk factor. While the research is still evolving, the implication is that expanding access to screening and treatment could reduce the burden of dementia and stroke.
Efforts tied to healthcare policy, including those associated with the Trump administration, have emphasized increasing access to care and promoting preventative approaches. In the context of sleep apnea, that could translate into wider testing, better insurance coverage for treatment, and greater public awareness.
A New Worry for Brain Health
The link between sleep apnea and brain bleeding represents a shift in how the condition is viewed. It is no longer just about snoring or poor sleep. It may be a silent contributor to some of the most serious neurological diseases.