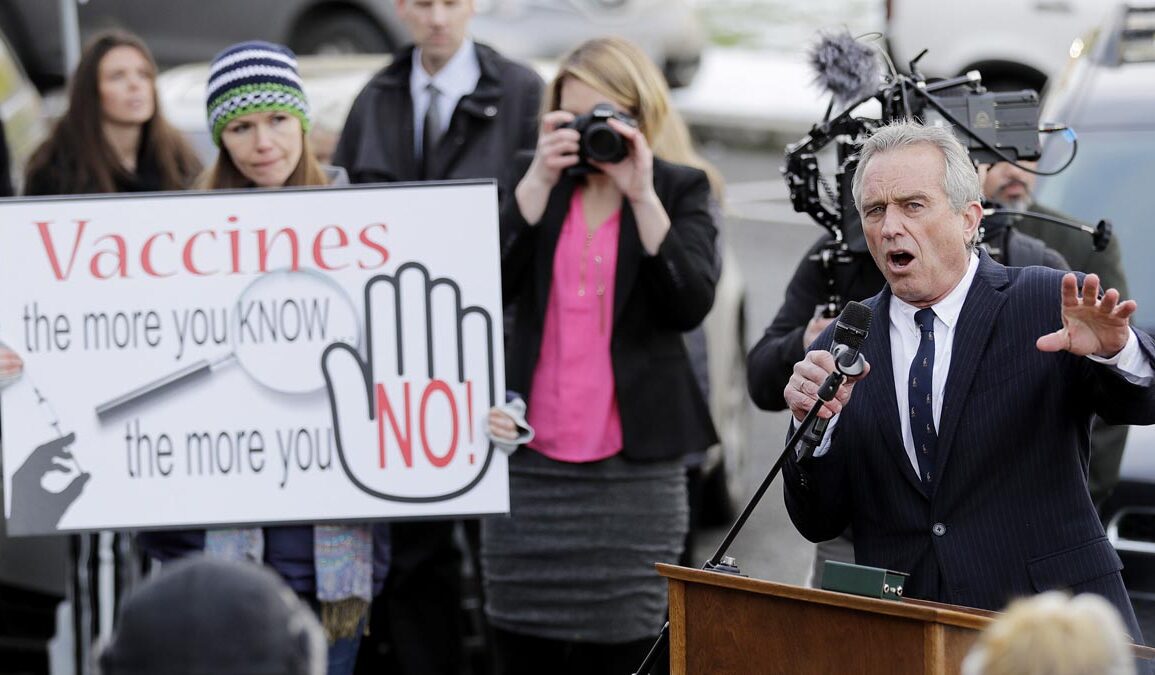A major shift in U.S. vaccine policy is now under review after a panel of experts selected by Health Secretary Robert F. Kennedy Jr. voted to recommend delaying the first hepatitis B vaccine dose for infants whose mothers test negative for the virus. The split vote signals that one of the earliest vaccines given to American babies may soon be pushed back by months.
Who RFK Jr. Is and What Panel He Convened
Robert F. Kennedy Jr., the current U.S. health secretary, appointed a new group of experts to the Centers for Disease Control and Prevention’s Advisory Committee on Immunization Practices. This panel, commonly known as ACIP, plays a central role in shaping the national vaccine schedule. The CDC usually adopts ACIP’s guidance, which can influence state vaccine requirements and medical practice across the country.
On Dec. 5, this panel voted to recommend that federal officials stop advising parents to vaccinate their newborns against hepatitis B immediately after birth unless the baby’s mother tests positive for the virus.
Which Vaccine Is Being Delayed and What the Panel Recommended
The recommendation focuses on the hepatitis B vaccine, which has long been given to nearly all U.S. infants within 24 hours of birth. ACIP now advises a different approach. For infants born to mothers who test negative for hepatitis B, the panel suggests that parents and health care providers make an individual decision on whether and when to vaccinate. If parents choose vaccination, the first dose should not be given before 2 months of age.
The existing recommendation remains unchanged for infants whose mothers test positive or whose hepatitis B status is unknown. Those babies should still receive the vaccine within 12 hours of birth.
Why Panel Members Say a Delay Is Needed
Supporters of the change argue that the scientific data behind the original policy is outdated and inadequate. Retsef Levi, a member of the committee, said the goal is to return to public health policy based on individual risk and informed consent. He told the panel that the current evidence is too limited to justify giving the vaccine to newborns who face extremely low risk of exposure. He described the existing data as outrageous and said he did not understand how federal officials could be confident in recommending the shot for infants immediately after birth.
Other experts raised concerns about the original clinical trials that supported the vaccine’s approval. Dr. Tracy Beth Hoeg, the acting director of the FDA’s Center for Biologics Evaluation and Research, pointed out that early trials had no control groups and monitored infants for only a week. She said such data would never meet today’s standards for vaccine approval.
Some members also noted that antibody levels decrease over time among those vaccinated at birth. They argued that if protection declines and infection rates were already falling before universal newborn vaccination began, a later dose could still be protective without exposing newborns to unnecessary risks.
Several doctors and public health organizations strongly opposed changing the schedule. Critics warned that delaying the first dose could lead to more children developing chronic hepatitis B infections. Former CDC Director Rochelle Walensky and two colleagues wrote that postponing the shot introduces risks with lifelong consequences and offers no measurable health benefit. A modeling study, though still a preprint, predicted more than 1,400 new chronic infections in the first year alone if the change is implemented.
Physicians who voted against the delay said abundant data show the vaccine is safe and effective. Dr. Cody Meissner argued that the sharp decline in hepatitis B cases since the early 1990s proves the benefit of the universal birth dose. James Campbell of the American Academy of Pediatrics called the recommendation very dangerous and warned it would put children at risk of infections that can lead to liver failure or cancer later in life.
Some experts also noted that testing during pregnancy sometimes misses infections or occurs too early, meaning a small but real number of infants may be unprotected if birth vaccination is no longer routine.
Why the Vote Matters and What Comes Next
The vote passed 8 to 3, but it is not final. The recommendation must be approved either by acting CDC Director Jim O’Neill or by Health Secretary Kennedy. If adopted, the national vaccine schedule will shift for the first time in more than 30 years on this issue.
This change would follow other recent adjustments made under Kennedy’s leadership, including removing the universal COVID-19 vaccine recommendation for children and revisiting other childhood shots. Critics claim these decisions undermine vaccine confidence. Supporters say they simply reflect a long overdue reassessment of vaccines that have not been thoroughly reviewed in decades.
For now, doctors, parents, policymakers, and vaccine manufacturers are preparing for what could be a major turning point in how the United States handles one of the first vaccines most children ever receive.