We constantly release clouds of volatile chemicals through our skin and breath. Researchers are learning that these scents can signal disease long before classic symptoms appear. From Parkinson’s and cancer to brain injuries and infections, body odor is becoming a serious diagnostic clue.
A Nurse Who Could Smell Parkinson’s
In Scotland, retired nurse Joy Milne noticed a new musky smell on her husband years before he was diagnosed with Parkinson’s disease. Scientists at the University of Edinburgh tested her by giving her 12 T-shirts, six worn by people with Parkinson’s and six by people without it. She identified all six patients and flagged one control who was diagnosed less than a year later. Her extraordinary sensitivity, called hereditary hyperosmia, helped launch a new wave of research into odor biomarkers.
What Illnesses Already Have Recognizable Scents
Some diseases are smelly enough for most people to notice.
- Diabetes during hypoglycemia can cause fruity or “rotten apples” breath because of ketones.
- Liver disease may produce a musty or sulfurous odor on the breath or in urine.
- Kidney disease can give breath an ammonia, fishy, or urine-like smell.
- Infections can carry signatures too. Sweet-smelling stool has been linked to cholera and C. difficile, though one study found nurses could not reliably diagnose by smell alone. Tuberculosis has been described as breath like stale beer and skin like wet cardboard and brine.
- Malaria research in Kenyan children found a “fruity and grassy” skin odor driven by aldehydes such as heptanal, octanal, and nonanal.
Beyond disease itself, normal factors change our scent. A comprehensive review finds that axillary odor varies with sex, age, ethnicity, emotions, personality, diet, climate, hygiene, and disease, and that microbes on the skin convert odorless sweat components into the volatile compounds we smell.
Dogs, Super-Smellers, and the Push to Digitize the Nose
Dogs have been trained to detect several cancers in urine or breath, including prostate, lung, breast, ovarian, and bladder cancers. In one prostate cancer study, trained dogs reached 99 percent detection on urine samples. Dogs have also shown promise for malaria, diabetes, epileptic seizures, and early Parkinson’s. Training is slow and not every dog qualifies, so researchers are building devices that can match canine noses.
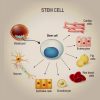
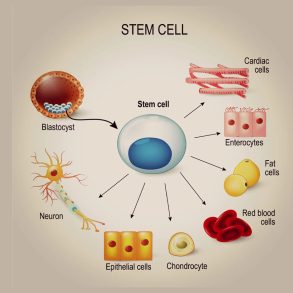
Physicist Andreas Mershin, co-founder of RealNose.ai, is developing a “robotic nose” for medical screening. His team grows human olfactory receptors from stem cells and uses machine learning to read their activation patterns from samples, with a focus on prostate cancer. As he puts it, the diagnostic “signal is already outside and detectable.”
How Scientists Read the Chemistry of Smell
Smells come from volatile organic compounds, or VOCs. Diseases disrupt metabolism, changing which VOCs evaporate from skin, sweat, urine, or breath. Researchers then separate and identify these molecules:
- Gas chromatography–mass spectrometry is being used by Perdita Barran’s team to analyze sebum from people with Parkinson’s. Of roughly 25,000 compounds found on human skin, about 3,000 shift in Parkinson’s, and her group has narrowed consistent differences to around 30, many of them long-chain lipids. The team is building a simple skin-swab test to triage patients earlier.
- In a Newsweek-reported mouse study from the Hefei Institutes of Physical Science, scientists used HS-SPME-GC-MS to screen VOCs for “pan-cancer” detection. Early tumor signals appeared in urine at week 5, in odor at week 13, and in feces at week 17, well before advanced disease.
- Bruce Kimball at the Monell Chemical Senses Center studies VOCs for multiple conditions and is developing a test for concussions in young athletes. His work has found specific ketones in human urine within hours after head injury, hinting at the brain’s effort to mobilize energy for recovery.
Why Armpits Matter: Sweat, Microbes, and Odor
Apocrine and eccrine sweat glands, along with skin bacteria, generate many signature smells. Bacteria convert sweat precursors into short-chain acids and sulfur-containing alcohols that define underarm odor. Genetics matter too. Variants in the ABCC11 gene are linked to stronger or weaker axillary odor, and different bacterial communities shape what we perceive.
Menopause and Body Odor Changes
Hormonal shifts in menopause can alter both scent and how smells are perceived. Hot flashes increase perspiration. Changes in estrogen and vaginal microbiota can affect genital odor. Stress and anxiety can raise apocrine “stress sweat,” which smells stronger because it contains more proteins and fats. These changes are usually benign, but persistent strong odors can signal infection and should be evaluated by a clinician.
Devices on the Horizon
Several technologies are racing from lab to clinic.
- Skin-swab Parkinson’s test: Barran’s team has identified a small panel of lipid-like compounds and aims for a quick, non-invasive triage test so patients reach neurologists sooner.
- Robotic noses: RealNose.ai is building an odor-detecting device using human olfactory receptors plus AI to pattern-match prostate cancer scent signatures.
- Sideline concussion screen: Kimball’s VOC assay for early post-impact ketones may aid rapid sports decisions.
- Malaria traps and tests: Replicating the fruity aldehyde blend could lure mosquitoes away from communities, and the same chemicals could underpin a noninvasive diagnostic.
What Experts Say About the Promise and Pitfalls
Supporters see a revolution in early detection. “What we want is to have a very quick, non-invasive test,” says Perdita Barran, so patients can be triaged effectively. Kimball notes that VOC differences between health and disease are common across many conditions. Abhinav Bhushan argues that if we can diagnose neurodegenerative disease early, we may slow or prevent progression.
Skeptics urge rigor. Richard Doty points out that doctors once used odor at the bedside, but modern diagnostics are more precise and many factors, from diet to age, confound smell. Thomas Hummel calls the work fascinating but stresses that many open questions remain. Even super-smellers like Joy Milne are rare and can only process limited samples, which is why repeatable lab methods and devices are essential.
Where This Could Lead
Odor science is moving from anecdotes to analytics. Panels of VOCs from skin, breath, urine, or stool could enable earlier, cheaper screening for Parkinson’s, concussions, malaria, and multiple cancers. Dogs and super-smellers proved that the signals exist. Now chemistry and machine learning are turning those signals into tests that any clinic could use.
Milne, who now collaborates with researchers, sums up the power of observation. Caregivers and families often notice changes first, including scent. Paying attention to those early clues, and capturing them with better tools, may help us diagnose sooner and treat more effectively.