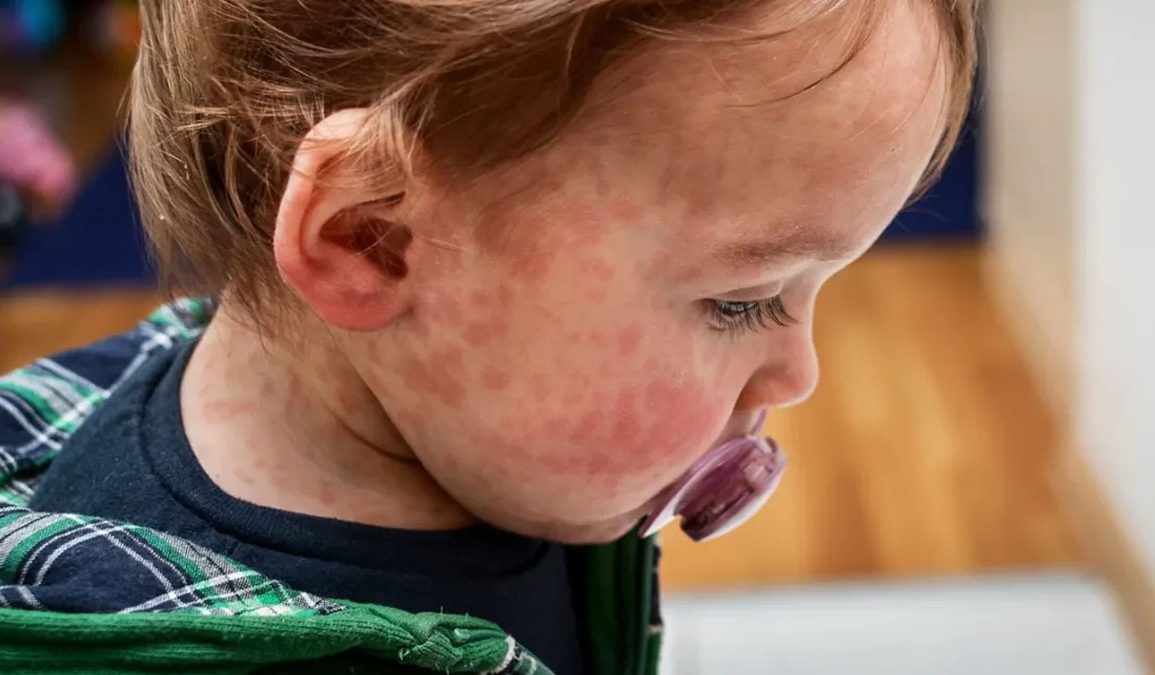
For years, many parents have assumed food allergies are mainly inherited. If a parent has allergies, the child will too. But a major new evidence review shows the story is more complex. Genes matter, but they are not the whole explanation. Early life exposures, skin health, the microbiome, and timing of first foods all play powerful roles.
The findings were published February 9, 2026, in JAMA Pediatrics. The research suggests that food allergy often develops from a combination of factors rather than from genetics alone.
The study was led by Nazmul Islam, Alexandro W. L. Chu, and senior researcher Dr. Derek K. Chu of McMaster University in Canada, along with a large international team. They conducted a systematic review and meta analysis of 190 studies involving about 2.8 million participants across 40 countries.
They examined 342 different risk factors to understand what increases the chances that a child will develop a food allergy before age 6. Only studies using proper food challenge testing were included to estimate how common food allergy truly is.
The researchers found that about 4.7 percent of children develop a food allergy by age 6. That is roughly 1 in 20 children.
Dr. Chu explained the big takeaway clearly. “Our study highlights that genetics alone cannot fully explain food allergy trends, pointing to interactions – or a ‘perfect storm’ – between genes, skin health, the microbiome and environmental exposures.”
This means that while inherited risk matters, the immune system is shaped by many early life experiences.
Major Risk Factors Beyond Genetics
The study identified several strong risk factors that are not purely genetic.
One of the strongest was eczema during the first year of life. Eczema was associated with nearly quadrupling the risk of food allergy. Allergic rhinitis and conjunctivitis tripled risk, and wheezing doubled risk.
Increased skin transepidermal water loss, which reflects a weakened skin barrier, was also strongly associated with food allergy. This supports the idea that damaged skin may allow allergens to interact with the immune system in ways that promote allergy.
Delayed introduction of allergenic foods was another major factor. Introducing peanut after 12 months was associated with more than double the risk of peanut allergy.
Antibiotic use was also important. Antibiotic use in the first month of life showed one of the strongest associations, roughly quadrupling risk. Antibiotic exposure during pregnancy or during the baby’s first year also increased risk, though more modestly, by about 32 to 39 percent.
The researchers classified these as major risk factors, especially when the odds ratio was 2 or higher and the absolute risk increase exceeded 5 percent.
Examples of How Food Allergies May Develop
The review supports several pathways through which food allergies may develop even without strong genetic predisposition.
A baby with early eczema may have a weakened skin barrier. Allergens that contact inflamed skin may trigger immune sensitization. Later, when the food is eaten, the immune system reacts strongly.
A newborn exposed to antibiotics in the first month may experience disruption of the gut microbiome. The microbiome plays a role in training the immune system. If that training is altered, the immune system may become more likely to misidentify harmless foods as threats.
If parents delay introducing peanut or egg beyond the first year, the immune system may not develop tolerance through early oral exposure. Later introduction may then carry higher risk.
Together, these pathways support what the authors describe as a multifactorial model rather than a single cause.
Factors That Did Not Show Important Risk Differences
The review also ruled out several suspected causes. Low birth weight, postterm birth, lack of breastfeeding, maternal diet during pregnancy, and maternal stress during pregnancy did not show important risk differences.
This is important because it helps narrow the focus to the most credible and consistent predictors.
How These Non Genetic Risks Can Be Addressed
The study did not test treatments directly, but it does point toward prevention strategies.
Identifying babies with early eczema or other allergic conditions can help clinicians recognize those at higher risk.
Avoiding unnecessary antibiotic use, especially in the first month of life, may reduce disruption of the infant microbiome.
Introducing allergenic foods such as peanut during infancy rather than delaying past one year may reduce risk.
The researchers said their findings could help identify babies at risk and “potentially ward them off through early prevention.”
Dr. Chu said, “This study has broadened our understanding of food allergies.”
He emphasized the need for better future research, stating, “Future studies should measure and adjust for the same key factors, include more diverse populations and use food challenge testing more often.”
He added that action is needed, saying, “New randomized clinical trials and updated guidelines are urgently needed to move our findings into action.”
Food allergy development is not determined by genetics alone. According to this large review of 2.8 million children, it is more accurate to view food allergy as the result of intersecting genetic, microbial, environmental, and immune factors.
Early eczema, antibiotic exposure, delayed introduction of allergenic foods, and other immune related conditions play major roles. Understanding these patterns may allow doctors and parents to better identify high risk infants and apply early prevention strategies.
In short, food allergies often arise from a convergence of influences, not just inherited DNA.